Sialolithiasis and its management in oral and maxillofacial surgery
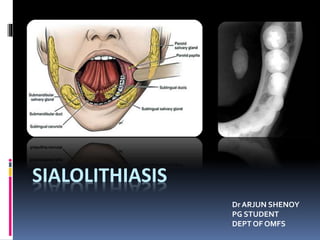
- 1. SIALOLITHIASIS Dr ARJUN SHENOY PG STUDENT DEPT OF OMFS
- 2. INTRODUCTION Sialoliths are calcified structures that develop within the salivary gland or the ductal system. Men > women Rare in children 75% - single 3% - bilateral 1.2% -autopsy
- 3. GLAND WISE DISTRIBUTION 80-92% - submandibular gland. 6-20% - parotid. 1-2% - sublingual and the minor salivary glands. Submanibular – larger & intraductal Parotid – multiple, within the gland
- 4. SUBMANDIBULAR GLAND OCCURENCE Abundant calcium concentration Alkaline Ph Anatomic factors Wharton’s duct - longest - two sharp curves - small punctum
- 5. Composition organic Inorganic Organic substances MUCOPOLYSACCHARIDES GLYCOPROTEINS CELLULAR DEBRIS
- 6. INORGANIC CALCIUM PHOSPHATE Fe Cu CALCIUM CARBONATE Mn
- 7. CHEMICAL COMPOSITION Chemical composition Microcrystalline apatite (Ca5[PO4]3OH) or Whitlockite (Ca3[PO4]) Brushite and weddellite BRUSHITE WEDDELLITE
- 8. RECENT DISCOVERIES Scanning electron microscopy has demonstrated oval, elongated shapes, suggesting the presence of bacilli in sialoliths. A recent polymerase chain reaction study found bacterial DNA, mainly belonging to the Streptococcus genus ARCH OTOLARYNGOL HEAD NECK SURG/VOL 129, SEP 2003
- 9. PATHOGENESIS Multifactorial event Secretory disturbances & precipitation – inflammatory process Specific changes in structure of organic molecules – supportive frame formation Metabolic disturbances – alkalinity & precipitation
- 10. MICROLITHS Concrements detectable only microscopically Contain – calcium and phosphorus hydroxyl apatite organic secretory material necrotic cellular residues Generated - autophagocytosis of organelles that are rich in calcium.
- 11. Dyschylia - Disturbed salivary secretion & change in the composition Accumulation of organic substances & mineralisation of organic matrix Accumulation of calcium Increase in pH Decreases the solubility of calcium phosphates
- 12. PROGRESSION Secretory disturbances viscous secretions Microlith formation ductal obstruction Coaction of factors + participation of bacteria sialoliths Dyschylia & increasing microlith formation ascent of bacteria lead to a focal obstructive atrophy of the acinar cells secretory disturbances Journal of Oral Science, Vol. 45, No. 4, , 2003
- 13. OTHER FACTORS Infection Salivary dysfunction Ductal anamolies Foreign bodies Ductal epithelium metaplasia
- 14. SYMPTOMS Pain, swelling & discomfort Pain - meal time – severe with sour or acidic food Unusual taste Associated with infection – fever , purulent discharge & lymphadenopathy
- 15. CHARACTERISTICS The annual growth rate - 1 mm per year Shape - round or irregular Size - 2 mm to 2 cm
- 16. GIANT SIALOLITH 72 mm in length and weighing 45.8 g The ability of a calculus to grow and become a giant sialolith depends mainly on the reaction of the affected duct. Rai and Burman. Giant Submandibular Sialolith. J Oral Maxillofac Surg 2009.
- 17. TREATMENT MODALITIES Newer treatment modalities - extracorporeal short-wave lithotripsy and sialoendoscopy are effective alternatives to conventional surgical excision for smaller sialoliths. However, for giant sialoliths, transoral sialolithotomy with sialodochoplasty or sialadenectomy remains the mainstay of management.
- 18. HISTOLOGIC FEATURES Stratified & mineralized with metaplastic excretory duct cells Concentric laminated structures Acini infiltrated by lymphocytes Dialatation of duct Epithelium exfoliation
- 19. DIAGNOSIS History Clinical examination Bi-manual palpation Imaging
- 20. BIMANUAL
- 21. IMAGING Conventional radiography Sialography Ultrasonography Computed tomography (CT) Magnetic resonance imaging (MRI) Sialoendoscopy Imaging
- 22. Conventional radiography Intra oral radiographs IOPA , Occlusal radiographs Extra oral radiographs Panaromic , PA skull projection Intraglandular and small stones can be missed. 20% of sialoliths are radiolucent
- 23. Sialography "Gold Standard” Retrograde infusion of oil or water based contrast & the architecture of the salivary duct system is visualized radio graphically .
- 24. LIMITATIONS Advantage detects radiolucent stones Therapeutic Disadvantage • invasive • bleeding & perforations contraindicated • acute infections • allergic to contrast
- 25. Ultrasonography Non invasive, alternative method Stones > 2mm detected as echo-dense spots with a characteristic acoustic shadow.
- 26. MR Sialography Non invasive Acute infections Canulation not possible
- 27. COMPUTED TOMOGRAPHY Posterior of the duct Hilum of the gland Substance of the gland Radiation exposure Non invasive & do not require contrast media
- 28. SIALOENDOSCOPY Minimally invasive Diagnostic & therapeutic Small endoscope – light at end of flexible cannula
- 29. Differential diagnosis Phleboliths – radiolucent center Dystrophic calcification of lymph nodes – Cauliflower shaped Palatine tonsiliths- multiple & punctate Haemangiomas with calcifications
- 31. • Opening of wharton’s duct Trans oral Ductotomy ( sialolithotomy) • Deep intra glandular • Multiple stones • Prevent recurrence Sialoadenectomy
- 32. Sialoendoscopy Small endoscope – optical fibres - irrigation or working ports Special devices – guide wire - balloon catheters - metal baskets - laser fibres Ductal dialation – lacrimal probe - balloon dialator
- 34. Sialoendoscopy – assisted Sialolithectomy Large sialolith Lithotripsy Fragmentation Types – intracorporeal - extracorporeal
- 35. Intracorporeal techniques Mechanical fragmentation Intracorpreal laser lithotripsy - Er: YAG - Ho: YAG Pneumatic lithotripsy
- 36. ARCH OTOLARYNGOL HEAD NECK SURG/VOL 129, SEP 2003
- 37. Extracorporeal Lithotripsy Shock waves – focused, multiple high intensity acoustic pulses Kinetic energy – compressive & tensile forces
- 38. Complications -Inability to remove fragment -Postoperative infections -Neural damage -Intraductal adhesion -Subglossal scar band formation -Sialocele & Ranula formation
- 39. paediatric patients Relatively small and distal Bimanual careful palpation is mandatory to diagnostic approach for children suspicious of sialolithiasis. These findings also suggest that intra-oral approach is effective treatment procedure for most of sialolithiasis in children. Int J Pediatr Otorhinolaryngol 2007 May;71(5)
- 44. Conclusion Sialolithiasis is the main cause of unilateral diffuse parotid or submandibular gland swelling. Mechanical obstruction of the salivary duct, causing repetitive swelling during meals, & often complicated by bacterial infections. Common in submandibular gland , 10 – 20% are radiolucent Newer minimally invasive diagnostic & therapeutic modalities
- 45. References Contemporary OMFS – Perterson Oral Radiology – principles & interpretation – White & Pharoah Sialoendoscopy & salivary gland sparing surgery - Oral Maxillofaccial Surg Clin N Am 21 (2009) Pathogenesis & diverse histologic findings of sialolithiasis – J Oral Maxillofac Surg 68: 2010 Imaging the major salivary glands – British Journal of Oral & Maxillofacial Surgery 49 (2011) Oral & maxillofacial pathology – Neville Text book of OMFS – Neelima Mallik
Editor's Notes
- cannot Do not fully explain the genesis of sialoliths.
