Cell Injury and Death Review
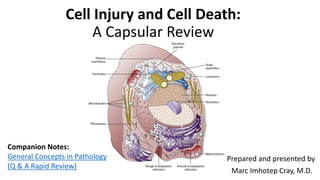
- 1. Cell Injury and Cell Death: A Capsular Review Prepared and presented by Marc Imhotep Cray, M.D. Companion Notes: General Concepts in Pathology (Q & A Rapid Review)
- 2. Marc Imhotep Cray, M.D. Discussion Outline Reversible Cell Injury Hydropic Swelling Intracellular Accumulations Cellular Adaptation Atrophy Hypertrophy Hyperplasia Metaplasia Dysplasia Irreversible Cell Injury Necrosis Apoptosis 2
- 3. PowerPoint General Pathology Concepts & Diseases_ A Global Overview eNotes IVMS General Pathology Lecture Notes.pdf Images IVMS-Gross Pathology, Histopathology, Microbiology and Radiography High Yield Image Plates.pdf WebPath Website http://www-medlib.med.utah.edu/WebPath/webpath.html Companion learning tools and resources:
- 4. Marc Imhotep Cray, M.D. Stages of cellular response to stress & injurious stimuli 4 Kumar V and Abbas AK. Robbins and Cotran Pathologic Basis of Disease 8th ed. Philadelphia: Saunders, 2014
- 5. Marc Imhotep Cray, M.D. Ultrastructural features of reversible cell injury 5 Endoplasmic reticulum (ER): cisternae of the ER are distended by fluid in hydropic swelling Mitochondria: In some forms of acute injury, particularly ischemia (lack of adequate blood flow), mitochondria swell Plasma membrane: Blebs of plasma membrane- that is, focal extrusions of cytoplasm Nucleus: reflected mainly by segregation of fibrillar and granular components of nucleolus These changes in cell organelles are reflected in functional derangements (e.g., reduced protein synthesis, impaired energy production) After withdrawal of stress that caused reversible cell injury, by definition, cell returns to its normal state Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013.
- 6. Marc Imhotep Cray, M.D. Reversible Cell Injury: Hydropic Swelling Cellular swelling in kidney tubule epithelial cells. A, Normal kidney tubule with cuboidal cells; B, early ischemic changes showing surface blebs and swelling of cells. Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 6
- 7. Marc Imhotep Cray, M.D. Reversible Cell Injury: Intracellular Accumulations Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 7 Intracellular accumulations may be categorized as (1) excessive amounts of normal intracellular substances such as fat (2) accumulation of abnormal substances produced by cell b/c of faulty metabolism or synthesis, and (3) accumulation of pigments and particles that cell is unable to degrade Lipids may contribute to atherosclerotic diseases and accumulate in blood vessels, kidney, heart, and other organs Fat filled cells tend to compress cellular components to one side and cause tissue to appear yellowish and greasy Fatty liver showing large intracellular vacuoles of lipid.
- 8. Marc Imhotep Cray, M.D. Reversible Cell Injury Roles of chaperone proteins in protein refolding and ubiquitin in protein degradation after stress-induced protein damage 8
- 9. Marc Imhotep Cray, M.D. Reversible Cell Injury Intracellular Accumulations (1) 9 Accumulations of silicon dust in tissues of the lung. Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. Excess accumulations of substances in cells may result in cellular injury b/c substances are toxic or provoke an immune response, or merely b/c they occupy space needed for cellular functions In some cases, accumulations do not in themselves appear to be injurious but rather are indicators of cell injury.
- 10. Marc Imhotep Cray, M.D. Reversible Cell Injury Intracellular Accumulations (2) 10 Intracellular accumulations may be categorized as: (1) excessive amts. of normal intracellular substances such as fat Abnormal metabolism as in fatty change in liver (2) accumulation of abnormal substances produced by cell b/c of faulty metabolism or synthesis Mutations causing alterations in protein folding and transport so that defective proteins accumulate Deficiency of critical enzyme responsible for lysosomal degradation (3) accumulation of pigments and particles that cell is unable to degrade an inability to degrade phagocytosed particles such as coal dust Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013.
- 11. Marc Imhotep Cray, M.D. Reversible Cell Injury KEY POINTS • Hydropic swelling is an early indicator of cell injury. It results from Na+- K+ pump dysfunction at cell membrane. • Intracellular accumulations of abnormal endogenous or exogenous particles indicate a disorder of cellular metabolism. • Damage from accumulation of abnormal intracellular protein is limited by chaperone proteins that attempt to refold the protein into its correct shape and by the ubiquitin-proteosome system that digests targeted proteins into fragments. 11
- 12. Marc Imhotep Cray, M.D. Cellular Adaptation Adaptive cellular responses of atrophy, hypertrophy, hyperplasia, metaplasia, and dysplasia Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 12
- 13. Marc Imhotep Cray, M.D. Cellular Adaptation (2) 13 A, Normal brain of a young adult. B, Atrophy of the brain in an 82- year-old male with atherosclerotic cerebrovascular disease, resulting in reduced blood supply. Kumar V and Abbas AK. Robbins and Cotran Pathologic Basis of Disease 8th ed. Philadelphia: Saunders, 2014.
- 14. Marc Imhotep Cray, M.D. Cellular Adaptation (2) A, Hypertrophy of cardiac muscle in left ventricular chamber. B, Compare with the thickness of normal left ventricle. This is an example of cellular adaptation to an increased cardiac workload. Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 14
- 15. Marc Imhotep Cray, M.D. Cellular Adaptation KEY POINTS • Adaptive cellular responses indicate cellular stress caused by altered functional demand or chronic sublethal injury. • Hypertrophy and hyperplasia generally result from increased functional demand. • Atrophy results from decreased functional demand or chronic ischemia. • Metaplasia and dysplasia result from persistent injury. 15
- 16. Irreversible Cell Injury: Necrosis Type of necrosis is dependent on nature, intensity and duration of injurious agent, and type of cell involved N.B.-initial membrane damage allows Ca+2 leakage with subsequent activation of Ca- dependent phosphatases and lipases Coagulative necrosis – cytoplasm of necrosed cells becomes eosinophilic and persists for many days (myocardial infarction) Liquefactive necrosis – cells undergo lysis rapidly (brain infarcts) Caseous necrosis – Mycobacterium tuberculosis interacts with macrophages Gangrenous necrosis – primary (bacterial toxins) or secondary (ischemia, infection) Fibrinoid necrosis – smooth muscle necrosis, fibrin release (malignant hypertension) Fat necrosis – inflammatory response to liberated fat fibrosis (pancreas)16
- 17. Irreversible Cell Injury: Necrosis (2) 17 There are also nuclear changes related to necrosis: Margination of chromatin chromatin condensing around periphery of nucleus o Chromatin clumping is reversible, but dissolution of entire nucleus is not reversible when nucleus is lost cell will die Pyknosis – small and dense nuclei Karyolysis – complete lysis of the nuclei Karyorrhexis – fragmented nuclei (generally seen in apoptosis)
- 18. Irreversible Cell Injury: Necrosis (3) 18 Irreversible cell injury is typically accompanied by: Release of intracellular enzymes: o Cardiac muscle – troponin, creatine kinase (MB isoform), aspartate (AST) transaminase, lactate dehydrogenase (LDH) o Hepatocytes – alanine transaminase o Striated muscle – creatine kinase (MM isoform) o Exocrine pancreas – amylase Loss of membrane selectivity – may be helpful in diagnosis through uptake of dyes Inflammatory response – initiated by products (mediators) of the necrotic cells
- 19. Marc Imhotep Cray, M.D. Coagulative necrosis / Dry gangrene Gangrene is a term used to describe cellular death involving a large area of tissue Gangrene usually results from interruption of major blood supply to a particular body part such as toes, leg, or bowel (ex. Diabetes mellitus patients) Depending on appearance and subsequent infection of necrotic tissue it is described as dry gangrene vs wet gangrene vs gas gangrene Dry gangrene is a form of coagulative necrosis characterized by blackened, dry, wrinkled tissue that is separated from adjacent healthy tissue by an obvious line of demarcation (as see in illustration) Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 19
- 20. Marc Imhotep Cray, M.D. Gangrene cont. Liquefactive necrosis may result in wet gangrene typically found in internal organs, appears cold and black, and may be foul smelling b/c of invasion of bacteria Rapid spread of tissue damage and release of toxins into bloodstream make wet gangrene a life-threatening problem Gas gangrene is characterized by formation of bubbles of gas in damaged tissue Gas gangrene is result of infection of necrotic tissue by anaerobic bacteria Clostridium perfringens o bacteria produce toxins and degradative enzymes that allow infection to spread rapidly through necrotic tissue Gas gangrene may be fatal if not managed rapidly and aggressively
- 21. Marc Imhotep Cray, M.D. Coagulative necrosis 21 Coagulative necrosis is most common Manifestations of coagulative necrosis are same, regardless of cause of cell death In general, steps leading to coagulative necrosis may be summarized as follows: (1) ischemic cellular injury leading to (2) loss of plasma membrane’s ability to maintain electrochemical gradients, which results in (3) an influx of calcium ions and mitochondrial dysfunction, and (4) degradation of plasma membranes and nuclear structures Two large infarctions (areas of coagulative necrosis) are seen in this sectioned spleen http://library.med.utah.edu/WebPath/CINJHTML/CINJ018.html
- 22. Marc Imhotep Cray, M.D. Coagulative necrosis (2) A. Normal heart. All myocytes are nucleated, and striations are clear. B. Myocardial infarction. The heart from a patient following acute myocardial infarction. The necrotic cells are deeply eosinophilic and most have lost their nuclei. Rubin R and Strayer DS Eds. Rubin’s Pathology: Clinicopathologic Foundations of Medicine, 6th Ed. Baltimore: LLW, 2012 22
- 23. Marc Imhotep Cray, M.D. Mechanisms by which ischemia leads to cellular death by necrosis 23 1. Loss of oxygen due to vascular occlusion impairs mitochondrial function resulting in decreased energy (adenosine triphosphate [ATP]) production by aerobic processes 2. Decreased ATP impairs ATP-dependent ion exchangers 3. Loss of aerobic processes causes anaerobic glycolysis to predominate, with consequent intracellular acidosis, eventually leading to increased cytosolic [Ca2+] 4. Ca2+-dependent phospholipases are then activated, causing loss of cell membrane integrity and necrosis Rubin R and Strayer DS Eds. Rubin’s Pathology: Clinicopathologic Foundations of Medicine, 6th Ed. Baltimore: LLW, 2012
- 24. Marc Imhotep Cray, M.D. Liquefactive necrosis When rate at which necrotic cells dissolve greatly exceeds rate of repair resulting appearance is termed liquefactive necrosis PMN cells of acute inflammatory reaction contain potent hydrolases capable of digesting dead cells A sharply localized collection of these acute inflammatory cells (generally in response to bacterial infection) produces rapid cell death and tissue dissolution Result is often an abscess a cavity formed by liquefactive necrosis in a solid tissue Liquefactivenecrosisinanabscessoftheskin. Rubin R and Strayer DS Eds. Rubin’s Pathology: Clinicopathologic Foundations of Medicine, 6th Ed. Baltimore: LLW, 2012 Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 24
- 25. Marc Imhotep Cray, M.D. Fat necrosis Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 25 Fat necrosis refers to death of adipose tissue usually results from trauma or pancreatitis Process begins with release of activated digestive enzymes from pancreas or injured tissue Enzymes attack cell membranes of fat cells causing release of their stores of triglycerides Pancreatic lipase can then hydrolyze triglycerides to free fatty acids and glycerol which precipitate as calcium soaps (saponification) Fat necrosis appears as a chalky white area of tissue
- 26. Marc Imhotep Cray, M.D. Caseous necrosis Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. 26 Caseous necrosis is characteristic of lung tissue damaged by tuberculosis Areas of dead lung tissue are white, soft, and fragile resembling clumpy cheese Dead cells are walled off from rest of lung tissue by inflammatory WBCs In center, dead cells lose their cellular structure but are not totally degraded Necrotic debris may persist indefinitely
- 27. Marc Imhotep Cray, M.D. Caseous necrosis (2) tuberculous lymph node 27 Hilar lymph node from a patient with active tuberculosis Irregular pink areas of caseous necrosis (arrow) are evident against a background of lymphocytes Inset: Granulomas on the periphery of necrotic areas show epithelioid macrophages and multinucleated giant (Langhans) cells (arrows) Rubin R and Strayer DS Eds. Rubin’s Pathology: Clinicopathologic Foundations of Medicine, 6th Ed. Baltimore: LLW, 2012
- 28. Marc Imhotep Cray, M.D. Apoptosis 28 Cell death can also occur through apoptosis it may be physiological deletion of selected cells (e.g. morphogenesis, cyclic hyperplasia of reproductive processes) or it may occur in response to a pathological stimuli Number of cells in tissues is tightly regulated by controlling rate of cell division and rate of cell death If cells are no longer needed they activate a cellular death pathway resulting in cell suicide Note: there are no gross structural changes involved with apoptosis
- 29. Marc Imhotep Cray, M.D. Apoptosis (2) 29 In contrast to necrosis, which is messy and results in inflammation and collateral tissue damage apoptosis is tidy and does not elicit inflammation Apoptosis is not a rare event large numbers of cells are continually undergoing programmed cell death as tissues remodel For example: During fetal development more than half of nerve cells that form undergo apoptosis It is estimated that more than 95% of T lymphocytes that are generated in bone marrow are induced to undergo apoptosis after reaching thymus
- 30. Marc Imhotep Cray, M.D. Apoptosis (3) 30 The initiation of apoptosis requires two processes: Priming – a reversible stage in which specialist machinery for apoptosis (e.g. transglutamase, calcium/magnesium endonucleases) are activated Triggering – the irreversible point which leads to a sustained rise in cytosolic calcium, and induction of new mRNA species for c-fos, c-myc and heat-shock proteins Apoptosis then proceeds: 1. Cytosol and nucleus lost half their volume 2. Fragmentation of nucleus and cytosol ( activation of transglutamase that forms an insoluble layer beneath the intact cell membrane) 3. Condensation of chromatin (pyknosis) 4. Macrophages bind to cell fragments prior to phagocytosis (non-specific mechanism)
- 31. Marc Imhotep Cray, M.D. Comparison of cellular changes in necrosis and apoptosis Copstead LC, Banksia JL. Pathophysiology, 5th Ed. St. Louis, Missouri: Saunders-Elsevier, 2013. Pathological cell death is more often due to necrosis process releases intracellular enzymes (useful diagnostically) and mediators that stimulate inflammation followed by healing by repair, scarring, contracture & distortion of tissue architecture
- 32. Marc Imhotep Cray, M.D. 32 IVMS General Pathology Lecture Notes.pdf
- 33. Marc Imhotep Cray, M.D. Necrosis and Apoptosis KEY POINTS • Necrosis occurs when the injury is too severe or prolonged to allow adaptation and is usually a consequence of disrupted blood supply. • Local and systemic indicators of cell death include pain, elevated serum enzyme levels, inflammation (fever, elevated WBC count, malaise), and loss of function. • Different tissues exhibit necrosis of different types: heart (coagulative), brain (liquefactive), lung (caseous), and pancreas (fat). • Gangrene refers to a large area of necrosis that may be described as dry, wet, or gas gangrene. Gas gangrene and wet gangrene may be rapidly fatal. • Apoptosis is cell death resulting from activation of intracellular signaling cascades that cause cell suicide. Apoptosis is tidy and not usually associated with systemic manifestations of inflammation. 33
- 34. Marc Imhotep Cray, M.D. 34 THE END Further study tools and resources on last slide.
- 35. Marc Imhotep Cray, M.D. Further study: 35 eLearning: IVMS General and Systems Pathology Cloud Folder Internet Pathology Laboratory for Medical Education http://library.med.utah.edu/WebPath/webpath.html#MENU Textbooks: Kumar V and Abbas AK. Robbins and Cotran Pathologic Basis of Disease 8th ed. Philadelphia: Saunders, 2014 Rubin R and Strayer DS Eds. Rubin’s Pathology: Clinicopathologic Foundations of Medicine, 6th Ed. Baltimore: Lippincott Williams & Wilkins, 2012
